Overview
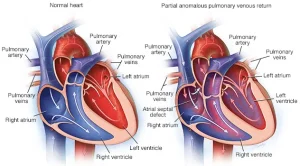
Partial Anomalous Pulmonary Venous Return (PAPVR) is a rare congenital heart condition in which one or more pulmonary veins do not connect normally to the left atrium of the heart. Instead, these veins connect to the right atrium or to veins that lead to the right side of the heart. Because of this abnormal connection, oxygen-rich blood from the lungs mixes with oxygen-poor blood, causing extra blood flow to the right side of the heart and the lungs.
In a healthy heart, all pulmonary veins carry oxygenated blood from the lungs directly to the left atrium so it can be pumped to the rest of the body. In PAPVR, only some of the pulmonary veins are connected incorrectly, while the others connect normally. The severity of the condition depends on how many veins are affected and the amount of extra blood flowing to the right side of the heart.
Some people with PAPVR may have mild symptoms or no symptoms at all, while others may experience complications over time if the abnormal blood flow places strain on the heart and lungs.
Symptoms
Symptoms of Partial Anomalous Pulmonary Venous Return vary depending on the size of the abnormal connection and the amount of blood being redirected. In mild cases, symptoms may not appear until later in life or may be absent entirely.
Common symptoms may include:
-
Shortness of breath, especially during physical activity
-
Fatigue or reduced exercise tolerance
-
Frequent respiratory infections
-
Heart palpitations
-
Mild chest discomfort
-
Bluish tint to the skin or lips in severe cases
-
Slow growth or poor weight gain in infants and children
Some individuals may be diagnosed during routine heart examinations or imaging tests performed for other reasons.
Causes
Partial Anomalous Pulmonary Venous Return occurs during fetal development when the pulmonary veins fail to connect properly to the left atrium. This abnormal development happens before birth and is present at birth.
The exact reason why this developmental error occurs is not always known. However, it is believed to involve abnormalities in the formation of the heart and blood vessels during early pregnancy.
PAPVR is sometimes associated with other congenital heart defects, especially atrial septal defect (ASD), which is a hole between the upper chambers of the heart.
Risk Factors
Because PAPVR is a congenital condition, risk factors are mostly related to factors that influence fetal heart development.
Possible risk factors include:
-
Family history of congenital heart defects
-
Genetic abnormalities affecting heart development
-
Maternal infections during pregnancy
-
Exposure to certain medications or harmful substances during pregnancy
-
Poorly controlled maternal health conditions such as diabetes
In many cases, however, PAPVR occurs without any identifiable risk factors.
Complications
If a significant amount of oxygen-rich blood flows to the right side of the heart due to PAPVR, the extra blood flow can place strain on the heart and lungs over time.
Possible complications include:
-
Enlargement of the right side of the heart
-
Pulmonary hypertension, which is high blood pressure in the lungs
-
Heart rhythm abnormalities
-
Heart failure in severe or untreated cases
-
Reduced oxygen delivery to the body
The risk of complications depends largely on how much blood is being redirected and whether other heart defects are present.
Prevention
There is currently no known way to prevent Partial Anomalous Pulmonary Venous Return because it develops before birth during the formation of the heart.
However, certain steps during pregnancy may help support healthy fetal development and reduce the risk of congenital heart defects in general.
Helpful preventive measures may include:
-
Receiving regular prenatal care
-
Avoiding alcohol, tobacco, and harmful drugs during pregnancy
-
Managing chronic medical conditions such as diabetes
-
Avoiding exposure to harmful chemicals or infections during pregnancy
-
Taking recommended prenatal vitamins, including folic acid
Early detection through medical imaging and regular health checkups can help ensure timely management and reduce the risk of long-term complications.
Advertisement