Overview
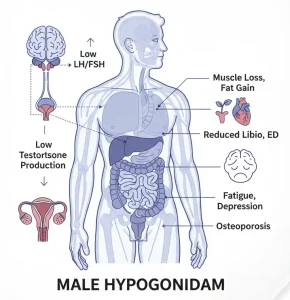
Male hypogonadism is a condition in which the body does not produce enough testosterone, the hormone responsible for male sexual development and reproductive function. It can also involve reduced sperm production or impaired testicular function. Testosterone plays a key role in maintaining muscle mass, bone density, red blood cell production, mood and sexual health. Male hypogonadism can develop at any age and may be present from birth or occur later in life due to illness, injury or aging.
There are two main forms of male hypogonadism. Primary hypogonadism occurs when the testicles do not function properly. Secondary hypogonadism occurs when the brain does not send proper signals to the testicles. Early diagnosis and appropriate treatment can help manage symptoms and reduce long-term health complications.
Symptoms
Symptoms of male hypogonadism vary depending on the age at which the condition develops and the severity of hormone deficiency.
In adults, symptoms may include:
-
Reduced sex drive
-
Erectile dysfunction
-
Fatigue and low energy levels
-
Loss of muscle mass and strength
-
Increased body fat
-
Decreased bone density
-
Mood changes such as depression or irritability
-
Difficulty concentrating
-
Reduced facial and body hair
If hypogonadism begins before or during puberty, symptoms may include delayed puberty, lack of deepening of the voice, reduced muscle development and poor growth of facial or body hair.
Causes
Male hypogonadism can result from a variety of conditions that affect the testicles, the pituitary gland or the hypothalamus.
Common causes of primary hypogonadism include:
-
Genetic conditions such as Klinefelter syndrome
-
Undescended testicles
-
Injury or trauma to the testicles
-
Chemotherapy or radiation therapy
-
Infections such as mumps affecting the testicles
Common causes of secondary hypogonadism include:
-
Disorders of the pituitary gland or hypothalamus
-
Tumors affecting hormone-producing areas of the brain
-
Chronic illnesses such as kidney or liver disease
-
Obesity
-
Certain medications, including opioids and steroids
-
Severe stress or rapid weight loss
Aging can also lead to a gradual decline in testosterone levels, sometimes referred to as late-onset hypogonadism.
Risk factors
Several factors can increase the risk of developing male hypogonadism, including:
-
Advancing age
-
Family history of genetic disorders affecting hormone production
-
Chronic medical conditions such as diabetes or HIV
-
Obesity
-
History of testicular injury or surgery
-
Long-term use of medications that interfere with hormone levels
Complications
If left untreated, male hypogonadism can lead to multiple health complications, including:
-
Infertility
-
Osteoporosis and increased fracture risk
-
Loss of muscle mass and strength
-
Increased risk of cardiovascular disease
-
Depression and reduced quality of life
-
Metabolic problems such as insulin resistance
Early identification and management can help reduce the risk of these complications.
Prevention
Not all cases of male hypogonadism can be prevented, especially those caused by genetic conditions. However, certain measures may help lower the risk or reduce severity:
-
Maintaining a healthy body weight
-
Managing chronic medical conditions effectively
-
Avoiding misuse of anabolic steroids or hormone-altering substances
-
Protecting the testicles from injury during sports or physical activity
-
Seeking medical advice for symptoms of hormone imbalance early
Regular health checkups and timely evaluation of symptoms can help ensure early diagnosis and appropriate treatment.
Advertisement